What is intra arterial tPA?
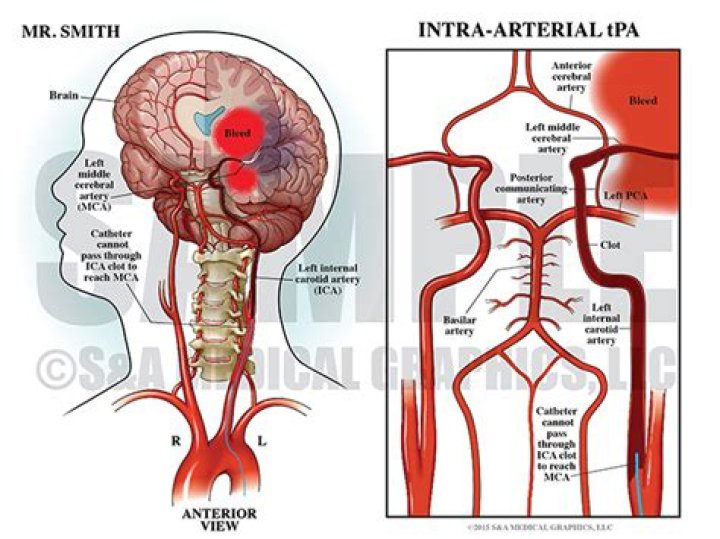
Besides, what is intra arterial therapy?
Abstract. Intra-arterial therapy (IAT) for acute ischemic stroke refers to endovascular catheter-based approaches to achieve recanalization using mechanical clot disruption, locally injected thrombolytic agents or both.
Likewise, what is the difference between tPA and TNK? The abbreviation “TPA” should not be used for written prescriptions or verbal orders for alteplase. Similarly, the abbreviation “TNK” should not be used to prescribe tenecteplase; the full brand name TNKase or full generic name tenecteplase should be used in written prescriptions and verbal orders.
Accordingly, what is tPA and how does it work?
TPA works by dissolving blood clots. That helps to restore blood flow to the brain after a stroke, potentially preventing additional brain cells from dying.
What is the window for administering tPA?
Currently, a new time window for tPA treatment in stroke has been proposed in that tPA can still be administered at 4.5 hours after stroke onset in certain eligible patients [2].
Related Question Answers
Is intra arterial?
Within an artery (blood vessel that carries blood from the heart to tissues and organs in the body).What is mechanical thrombectomy stroke?
With mechanical thrombectomy—also called endovascular therapy—a special device is threaded through the blood vessels to the site of a stroke-causing blood clot in the brain. The device grabs the clot and removes it, restoring blood flow to the brain—and dramatically improving outcomes.What is endovascular therapy for stroke?
Endovascular treatment of stroke is the non-surgical treatment for the sudden loss of brain function due to blood clots. The treatment uses microcatheters (thin tubes visible under X-rays) which are inserted into the blood clot from the groin or the arm.What is endovascular thrombectomy?
An endovascular thrombectomy is the removal of a thrombus (blood clot) under image guidance. A thrombectomy is most commonly performed for an arterial embolism, which is an arterial blockage often caused by atrial fibrillation, a heart rhythm disorder.What are side effects of TPA?
- A Skin Rash.
- Bleeding Gums.
- Bruising.
- Fever.
- Hives.
- Nausea.
- Nosebleed.
- Vomiting.
What happens if TPA is given too slow?
Conclusion: Because of its short half life, TPA should be administered as a bolus followed by an immediate infusion. Bolus to infusion delays or interruptions in the infusion of TPA after the bolus may significantly impact serum TPA levels and may reduce the efficacy of thrombolysis.Why is TPA given within 3 hours?
The timing of treatment is important, because giving a strong blood thinner like tPA during a stroke can cause bleeding inside the brain.How quickly does tPA work?
The half-life of tPA in the bloodstream is rather short, 5-10 minutes in humans, as a result of PAI-1-mediated inhibition and LRP1-mediated liver uptake [14].What happens in the first 3 days after a stroke?
During the first few days after your stroke, you might be very tired and need to recover from the initial event. Meanwhile, your team will identify the type of stroke, where it occurred, the type and amount of damage, and the effects. They may perform more tests and blood work.When should you not give tPA?
Relative Exclusion CriteriaPregnancy. Seizure at the onset with postictal residual neurological impairments. Major surgery or serious trauma within prior 14 days. Recent GI or urinary tract hemorrhage (within previous 21 days)
What happens after TPA is given?
TPA treatment has risks. There is approximately a 3% chance of symptomatic bleeding (symptomotic hemorrhage) into the brain (because TPA thins the blood) compared to 0.2% if TPA is not given. If bleeding into the brain happens after TPA is given, it may cause your stroke symptoms to be worse and may result in death.What are the two main types of stroke?
Types of Stroke- Ischemic Stroke (Clots) Occurs when a blood vessel supplying blood to the brain is obstructed.
- Hemorrhagic Stroke (Bleeds) Occurs when a weakened blood vessel ruptures.
- TIA (Transient Ischemic Attack) Called a “mini stroke,” it's caused by a serious temporary clot.
- Cryptogenic Stroke.
Is TPA a blood thinner?
It has also been used in treatment for pulmonary embolism and myocardial infarction. TPA is a blood thinner, and therefore it is not used for hemorrhagic strokes or head trauma.Is tenecteplase a tPA?
Tenecteplase (sold under the trade names TNKase and Metalyse) is an enzyme used as a thrombolytic drug. Tenecteplase is a tissue plasminogen activator (tPA) produced by recombinant DNA technology using an established mammalian cell line (Chinese hamster ovary cells).What drugs are thrombolytics?
The most commonly used clot-busting drugs -- also known as thrombolytic agents -- include:- Eminase (anistreplase)
- Retavase (reteplase)
- Streptase (streptokinase, kabikinase)
- t-PA (class of drugs that includes Activase)
- TNKase (tenecteplase)
- Abbokinase, Kinlytic (rokinase)